C.S. Lewis, the famous Christian author of the popular Chronicles of Narnia series, is given credit from having said “Experience: that most brutal of teachers. But you learn, my God do you learn.” It doesn’t take long living here on earth to appreciate the truthfulness of this remark. Books teach us. Professors teach us. There are life-lessons to be gathered from virtually every interaction we engage in. But nothing teaches like experience. I have found this to be true as a pharmacist. There is something you learn about medicine and patient-care from the experience of it in your life that simply cannot be obtained just from observation.
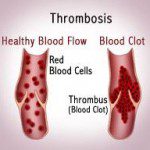
Last week I got a call from my mother. My parents are in their 70’s and live nearby. She had brought my father to the doctor due to some swelling in his ankle. My father, by the way, has advanced Alzheimer’s disease. His ankle/calf swelling was not totally unusual for him. It happens from time to time, possibly related to a broken leg many years ago. It typically would go down in a few days. This time it didn’t, and he seemed to be in some discomfort (not always easy to identify in an Alzheimer’s patient). They did an ultrasound. It was a DVT (deep vein thrombosis). Basically…a blood clot in his lower leg. These can be dangerous, though the risk of a Pulmonary Embolism (PE) is lower for distal clots (below the knee).
You should know the symptoms of a DVT. Not every DVT has symptoms like these. But since these symptoms might be mistaken for other problems, it is good to bear them in mind. Here they are, borrowed from Bayer’s website on thrombosis:
Clinical symptoms of DVT include swelling, pain, and discoloration of the affected extremity. Physical examination may reveal calf tenderness, unilateral edema, warmth, skin discoloration, and superficial venous dilatation. However, many of these signs and symptoms can occur in other conditions and therefore have a low predictive value for diagnosing DVT.
After traveling from the MD’s office to the emergency room my parents were initially told that another Ultrasound was going to be necessary and that they couldn’t use the one already done. Why? I’m not sure. At this point I was still at home, waiting to see where they would end up so I could meet them there. Not long after this I got a call that they would be administering Lovenox and sending them home with a prescription for Lovenox & Coumadin. I headed to the ER to meet them and offer my help.
The ER was crowded, and I found my parents sitting in the hallway waiting for someone to come and take some blood. While waiting a nurse came and demonstrated her technique for giving Lovenox. It was, I thought, a little unusual. She recommended a sort of clockwise injectable pattern around the belly button (at least 2 inches away). I’m more of a traditional “love handles” guy. But that’s fine. I’m not one to quibble over such things. But I’ll give it my way when we get home.
But one thing I noticed while waiting in the ER: I didn’t see any emergencies. Seriously. No bleeding wounds, no unconscious patients, no screaming. I’m not a total stranger to ER’s. And I know that many “emergencies” do not necessarily “look” like emergencies. But this has been my typical impression. This was my second lesson:
 LESSON 2: I think we have an ER problem
LESSON 2: I think we have an ER problem
People are being encouraged to use the ER for non-emergencies. I just read an article the other day about a new system being introduced to actually allow patients to make appointments for their ER visit. Make appointments? Yes. It’s like call-ahead seating at a restaurant. This trend enforces the idea that the ER can be used for routine concerns. Dr. Dino Rumoro of the American College of Emergency Physicians sees this as a problem. He said “An emergent condition is an emergency condition and it’s not subject to booking an appointment. It means you need to be seen right away.”
I’m aware of the JAMA article published recently suggesting that the “ER overuse” problem might be exaggerated. But the point of that study was intended more to expose the impropriety of insurance companies refusing payment based on discharge diagnoses. That’s fine. But the fact remains, as has been shown in other studies that “an estimated 56 percent of all emergency department visits are avoidable.“
We waited for the blood work, and I took the prescriptions for Lovenox and Warfarin to get them filled. I met my folks at home and we worked out a plan for me to give my father the injections twice daily for the next 5 days while the Coumadin kicks in.
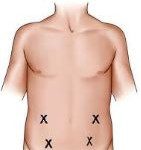 LESSON 3: Lovenox injections are pretty easy
LESSON 3: Lovenox injections are pretty easy
For those who may be concerned that giving themselves or a loved one this injection, let me assure you: you can do it. The shots are given into the fatty tissue on the sides of your abdomen. Follow the instructions given by your physician. Here are the basics:
-
Wash your hands with soap and water and then clean the injection site with an alcohol pad
-
Grab a pinch of skin around the “love handle” area on the left or right side and insert the needle STRAIGHT in. Then slowly inject the medicine.
-
Remove the needle STRAIGHT out and then, pointing it in a safe direction, press the plunger down firmly to activate the shield.
-
Usually there will be no blood and no pain. Discard the needle in a hard, disposable container.
For a great video tutorial, CLICK HERE.
So those are a few things this whole event has taught me – and maybe now – taught you.
Oh, and by the way, my father is doing just fine.
DVT Emergency Room Overuse Lovenox
Last modified: April 17, 2023